Solace Blog
- Activities19
- Autism & Behavioral4
- Community154
- Early Intervention71
- Events & Giving Back20
- Extraordinary Kids22
- Family Caregiver4
- Home Care Therapy60
- News92
- Parent Articles83
- Patient Testimonial21
- Pediatric Therapy76
- Pediatric Therapy Career46
- Private Duty Nursing1
- School-Based Services1
- Telehealth Therapy27
- Tips & Advice66

From School To Home: Christian’s Shift To Impactful Therapy
Speak, Listen, Connect: 6 Communication Strategies for Therapists
Your 5-Minute Mindfulness Break: 5 Simple Ways to Recharge Between Therapy Sessions
The Transformative Power of Occupational Therapy: Peter Leypold’s Journey
Connecting Hearts and Homes: A Deep Dive into Pediatric Home Health with Solace Pediatric Healthcare

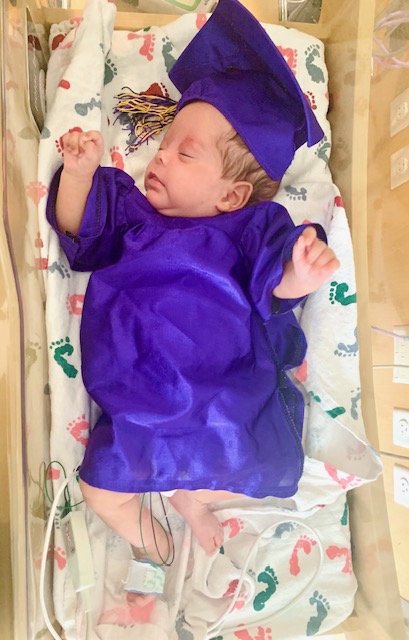
Infant Diagnosed With Periventricular Leukomalacia Discharged From PT
One-year-old Charlotte was born at 26 weeks of gestation and suffered a brain bleed a few days after her birth. Periventricular Leukomalacia (PVL) is an injury to the brain that often affects extreme preemies. Babies with PVL generally have no outward signs or symptoms of the disorder, but they are at risk for:
- Motor disorders
- Delayed cognitive development
- Coordination problems
- Vision and hearing impairments
There is no specific treatment for PVL. Treatment is symptomatic and supportive. The outlook for individuals with PVL depends upon the severity of the brain damage. Some children exhibit fairly mild symptoms, while others experience significant disabilities.
“We were told that it was minor, but that once the damage occurred, the decayed white matter in the brain would never regenerate or be repaired, said Romina, Charlotte’s mother.
“We were so afraid and already facing a long journey in the NICU. We didn’t know what this meant for her future. The worst part is that they couldn’t tell us exactly what would happen to her because the effects are usually seen around the child’s first or second birthday when they can identify the delays in their development.”
“During our journey in the NICU, we learned that early intervention was very important and it increased her chances of reaching her potential and hopefully help her catch up by the time she would be two-years-old,” added Romina.
Plan of Care
There are several treatment options available to manage physical, neurological, and cognitive symptoms caused by PVL. These treatment options aim to relieve pain and improve quality of life. Treatment options to manage periventricular leukomalacia symptoms include occupational therapy, physical therapy, feeding therapy and speech therapy.
As soon as Charlotte was discharged after 108 days in the NICU, Romina initiated the process to receive early intervention in their home. The therapists at Solace Pediatric Healthcare identified that Charlotte was 75%-80% delayed in comparison to full-term babies her age. As Charlotte got closer to her first birthday, her pediatrician recommended more therapy with Solace Pediatric Healthcare.
The initial plan was for Charlotte to receive feeding therapy to assist in gaining weight and to increase her intake of milk and puréed foods. In addition to feeding therapy, Ali, speech-language pathologist, also worked with Charlotte in combining words and increasing her expressive language skills.
Charlotte was referred to Solace Pediatric Healthcare for physical therapy due to a delay in motor skills. She was not rolling over on a consistent basis and she was not showing any signs of starting to crawl. The plan was to build strength to crawl even though she was at an age where she should’ve been starting to walk.
Collaborative Sessions
“Nicollette, the physical therapist, always had a plan for the goals we were working on. For crawling she would use physical guidance to teach Charlotte the movements and motion of crawling until she got strong enough to do it on her own. And when we moved on to walking she would have her first stand against sturdy furniture then walk towards me or her. And for climbing stairs Nicollette would use a toy to get her to go up and down with crawling then eventually standing while holding the railing. We were always so amazed whenever she reached a goal,” said Romina.

“Nicollette was always very energetic and enthusiastic when she arrived at our home. And even when Charlotte had a hard time and did not want to participate and only wanted me to carry her, Nicollette would find something interesting and fun to get her to be motivated and do the exercises. Our entire family was very impressed with her professionalism and knowledge about her field,” added Romina.
Telehealth Benefits
The pediatric telehealth clinicians at Solace Pediatric Healthcare specialize in virtual sessions and provide the same level of outstanding outcomes our children and families receive from our in-home sessions. Pediatric telehealth therapy removes the barriers of remote locations, weather, compromised immunities and challenging family schedules hindering many children from receiving individualized one-on-one care.
“I loved how interactive telehealth was with Charlotte, and how Nicollette always included me in the exercises for the sessions to make it fun. My in-laws were also included during therapy which they really enjoyed,” said Romina.

“From my husband, to my in-laws, to our sisters, we were all involved in Charlotte’s sessions and overall progress. Each therapist took the time to explain what the goals were at the time, and always left us with homework to do on our own which my husband enjoyed doing with Charlotte,” added Romina.
Charlotte will turn two-years-old in April, and she is already walking, running and jumping now!
“Our experience with Solace has been extremely positive. All the therapists have been very knowledgeable, reliable and professional. We were able to have the same team for over a year, which is often difficult in this field. And more importantly, they really cared about our daughter’s future and helping her reach her greatest potential,” said Romina.
How to Refer Your Child
Solace Pediatric Healthcare is the leading provider of family caregiver, occupational, physical, speech and feeding therapy services. Since 2005, our clinicians have provided pediatric care to children from birth to 21 years of age. We offer comprehensive pediatric therapy services in Colorado and Arizona.
At Solace, we’ve instilled a culture built on trust, communication, teamwork and accountability. Our mission is to provide pediatric clinical services to help children and families live their best lives.
- I want to refer my child for an Evaluation/Therapy. If you know you would like to speak to our patient advocate to discuss scheduling an initial evaluation with a licensed pediatric therapist, simply complete and submit the Referral Form so we may contact you. Please provide as much information on the secure/encrypted form as possible as it is required to begin the process. We do accept Medicaid and most insurances.
- I Want to Be Contacted. If you would like to speak with our patient advocate for more information prior to submitting a Referral Form, simply complete the Contact Me Form and submit.
- If you prefer to contact us to discuss your child, please call our team. You can reach us by phone at: (Denver) 303.432.8487; (Colorado Springs) 719.623.5463; (Northern Colorado) 970.775.8476; and (Pueblo) 719.695.4535.
Reference: National Institute of Neurological Disorder and Stroke
Share this Post